Survey of 1,000 women finds most were dismissed by a provider, most needed multiple providers to get an answer, and most weren’t prepared by school-based s
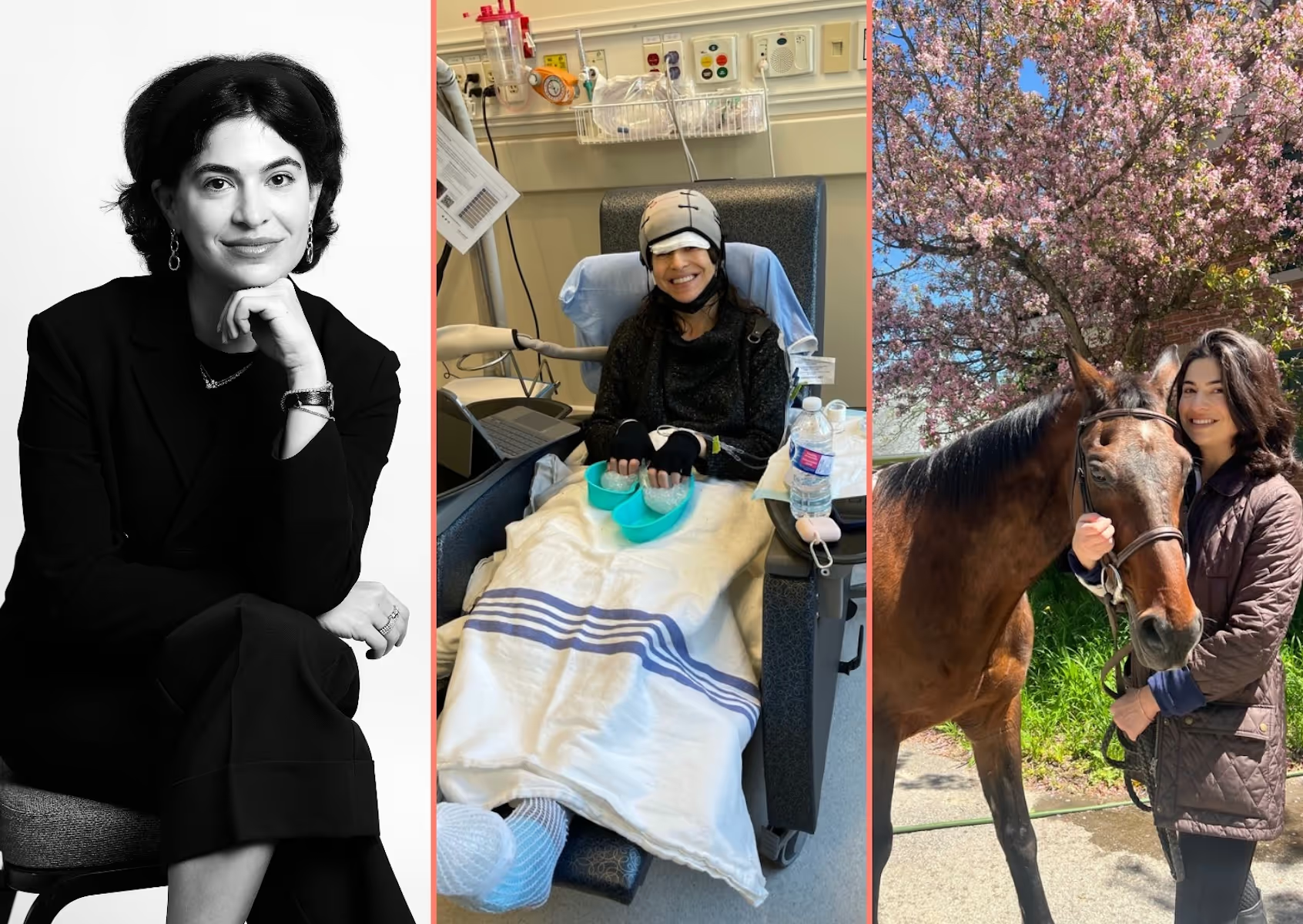
When Robby Spring was diagnosed with breast cancer, she faced decisions no one should have to make in a rush: about her body, her future, and her fertility. In the middle of navigating treatment, she also had to navigate identity loss, fertility preservation, and the emotional fallout that comes with both.
Instead of staying silent, Robby began sharing what she wished she had found during her own experience: real, honest content on what it means to go through cancer as a young woman and what fertility preservation actually looks and feels like. Whether it's advocating for more compassionate healthcare, helping others feel less alone, or creating the kind of support she needed herself, Robby is turning a life-altering diagnosis into something meaningful. We're so grateful to her for opening up about this part of her journey.

I was diagnosed with breast cancer at 35, and like so many young women, I had to make big decisions about my body, my treatment, and my fertility—fast. It was overwhelming and isolating. I come from a background in health and life sciences, but nothing prepared me for what it felt like to actually be the patient. I started sharing my story online to offer the kind of real, honest content I couldn't find when I needed it most. Now, I use my voice to push for better care and innovation in our healthcare system and to elevate the role of lived experience in oncology.
It came almost immediately. One of my first thoughts after being diagnosed was, oh my God, what is this going to mean for my fertility? I was 35, single, and suddenly facing decisions I never thought I'd have to make. I called a friend who's a gynecologist right away, and she helped me process what was ahead. From there, I was quickly referred to my own gynecologist, who immediately recommended I speak with a fertility clinic. I moved through the process faster than most, which I now realize was a privilege. Many patients don't get that kind of timely support.
I was given clear information at my appointments, but I had already taken matters into my own hands. I asked the right questions early and got referred. I know that's not the case for everyone. I was lucky—the hospital I was treated at works closely with the fertility clinic I ended up using, and I saw an oncofertility specialist who was absolutely amazing. But I also recognize that this kind of coordinated care isn't something all patients receive, and it shouldn't be up to the patient to figure it out on their own.
I had actually frozen my eggs selectively about a year and a half before my diagnosis, and that first experience was really tough, physically and emotionally. I didn't get as many eggs as I had hoped, and I didn't feel supported by the clinic I went to. So when I was referred to a new fertility clinic after my cancer diagnosis, I was pretty skeptical about doing it all over again.
But the doctor I saw specialized in oncofertility, and she was incredible. She explained that, as an oncology patient, there was some provincial coverage (Ontario) available. More importantly, she told me plainly: breast cancer can affect fertility, and I had a small window right now—I might not get another. She made me feel safe and seen, and that gave me the confidence to go through it again.
The process itself was still hard. I was in limbo, waiting for cancer treatment, full of fear and uncertainty. Egg freezing is physically intense, and I felt awful through much of it. But this time, the outcome was better, and I genuinely felt cared for. Looking back, I'm really glad I did it right away. It was taxing, but now I have a sense of certainty and peace that I wouldn't have had otherwise.
It wasn't easy. I ended up waiting 11 weeks from diagnosis to the start of treatment—which was far too long. But as more breast cancer spots were found and delays became inevitable, I realized I had a small window. My oncofertility doctor urged me to use that time for egg freezing, and thankfully, it worked out. Not everyone gets that kind of timing or support, and I'm grateful I was able to make it happen.
My biggest support systems were my friends and family. Just having someone walk with me outside, like my best friend did, made a huge difference in getting through the hardest days. That period was complicated—I went through a breakup and moved out of my ex's place the day after my egg retrieval. So while I didn't have support from a partner, I was lucky to be surrounded by people who showed up for me, and to have a medical team I trusted. I always encourage others to lean on those who genuinely care. You shouldn't have to go through something like this alone.
Honestly, I don't think there were any questions I didn't ask. I had gone through fertility preservation before, so I knew what to expect and made sure to ask everything I needed. I also had a great care team and made sure my doctor was really involved, which made a big difference. My advice to others would be: don't hold back. You deserve to feel confident during the process and cared for.
I feel incredibly lucky that these options exist—it gave me a sense of control at a time when everything felt uncertain. In some ways, it took pressure off aging and future timelines. But it also made me really sad. The spontaneity of having children might not be there for me, and the reality that these frozen eggs could be my only path to a biological child is heavy. There's grief in that. Now, being on the other side, I do feel some relief knowing I've taken steps to preserve my fertility. The emotional weight of it all is still very real, but I no longer feel defined by a ticking clock.

Social media didn't play a big role during my own treatment—I just couldn't find the kind of real, honest content I was looking for. Most of my support came from my personal network and friends of friends who had been through something similar. One exception was Rethink Breast Cancer, whose advocacy group supported me in meaningful ways.
But that gap I felt online is exactly what inspired me to start sharing my story. I launched my Instagram and TikTok accounts to support women going through oncofertility, post-chemo hair regrowth, and everything in between. Creating that space has become a huge part of my healing. There's still such a huge need for better tools and content that speak directly to young women facing these decisions—which is why I'm also excited about emerging platforms like myStoria that aim to bridge that gap even further.
You are not alone. So many women are navigating this, even if it doesn't always feel that way. Now is the time to ask all the questions and advocate for what matters to you. If fertility is a priority, make sure your healthcare team knows that—and don't hesitate to reach out to others who've been through it.
Make decisions for your future self, not just the overwhelmed version of you in this moment. When you're in crisis, it's easy to choose the path of least resistance, but sometimes the harder path is the one that gives you peace later on. Think about what the future version of you will want, and let her guide you.

Life after fertility preservation feels lighter in many ways. I have a deep sense of gratitude and confidence knowing I made that decision at the start of my cancer treatment. I was diagnosed with estrogen-positive breast cancer, went through chemotherapy, and was placed into chemical menopause. I'm now on hormone blockers for at least five years, so I knew these treatments would have lasting consequences on my ability to conceive naturally.
Preserving my fertility gave me a sense of security in the face of so much uncertainty—a way of protecting a piece of my future at a time when everything felt like it was being taken away. Today, I'm still single and focusing on healing, joy, and building a life that feels like mine again. What matters most is that I had the choice. And I hope every woman in this position is given the same opportunity to make informed, empowered decisions about her future.